Eating Your Way to Liver Health: Plant-Based Diet Can Shield You from Fatty Liver Disease
Have you ever stopped to ponder the intricate relationship between what we eat and how long we live? The concept of using food as medicine, while ancient, is experiencing a renaissance in the modern age. Among the most celebrated dietary approaches is the plant-based diet, a nutritional philosophy rooted in the profound impact of plant-derived foods on our health.
The Essence of a Plant-Based Diet
A plant-based diet, as the name suggests, centers around foods primarily derived from plants – fruits, vegetables, legumes, nuts, seeds, and whole grains. While plant-based diets can include small amounts of animal products, the emphasis is firmly placed on the consumption of plant foods. This approach isn’t just about following a trend; it’s a lifestyle choice rooted in science, compassion, and a commitment to better health.
The Benefits of Plant-Based Eating
The advantages of embracing a plant-based diet are manifold:
-
Heart Health: A diet rich in plant foods has been associated with a reduced risk of heart disease. It can help lower blood pressure, reduce cholesterol levels, and promote overall cardiovascular well-being.
-
Weight Management: Plant-based diets often support healthy weight management due to their lower calorie density and higher fiber content. This can help maintain a healthy body weight.
-
Cancer Prevention: Certain plant foods are rich in antioxidants and phytochemicals that may help protect against various types of cancer.
-
Digestive Health: The abundance of dietary fiber in plant-based diets can support healthy digestion and reduce the risk of digestive disorders.
-
Diabetes Control: Plant-based diets have been shown to improve blood sugar control and insulin sensitivity, making them a valuable tool in managing diabetes.
-
Chronic Kidney Disease: Foods rich in animal fat can cause acid buildup in the body that can lead to the progression of chronic kidney disease. A diet that is predominantly plant-based can help reduce this risk.
-
Environmental and Ethical Benefits: Plant-based diets have a lower environmental footprint and are often chosen for ethical reasons, such as animal welfare and sustainability.
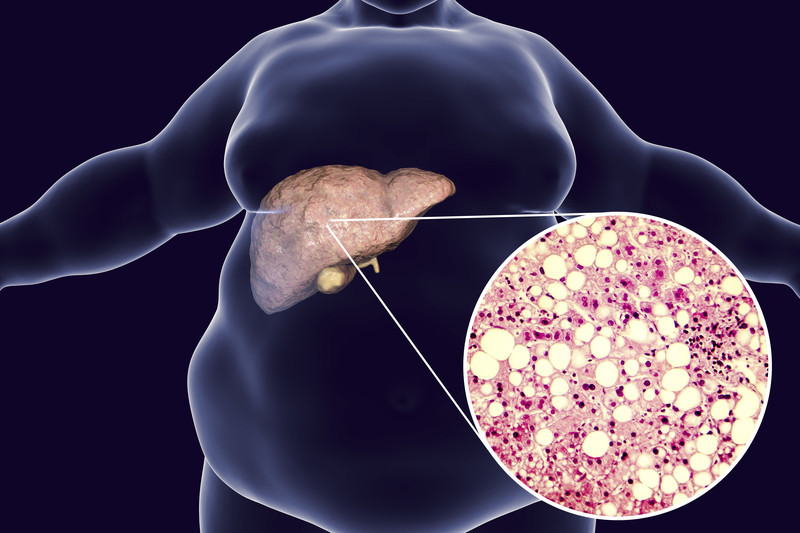
Fatty Liver Disease: A Silent Epidemic
Fatty liver disease (FLD) might not be a household name, but it’s becoming increasingly common, affecting about 30% of the global population. Its prevalence is growing globally at an alarming pace. FLD, which is more recently known as metabolic dysfunction-associated steatotic liver disease (MASLD) is a condition where excess fat accumulates in the liver, potentially leading to liver damage. For the purpose of this article, we will use the term FLD as it is a lot more commonly used term. Fatty liver disease (FLD) is a growing health concern, characterized by the accumulation of fat in the liver cells. This condition, often symptomless in its early stages, can progress to severe liver damage, leading to cirrhosis and liver-related complications.
Why FLD Deserves Our Attention
Fatty liver disease is not to be underestimated; it is intricately linked to lifestyle and dietary choices. Research shows that while genetics play a role, diet can significantly influence the development and progression of FLD. As highlighted in the introductory blog, the interaction between our genetics and the food we consume is crucial. A balanced, plant-based diet rich in essential nutrients and devoid of harmful components can mitigate the risk and impact of FLD, ultimately contributing to a longer, healthier life.
While genetics does play a role in FLD, a recent study suggests that the foods we eat, particularly plant-based foods, can be powerful allies in the fight against this condition. Plant-based diets will emerge as a key player in the endeavor to unlock the secrets of longevity and well-being. Let’s take a closer look at this groundbreaking research.
FLD and the Role of Diet.
Fatty liver disease is a result of a complex interaction between genetic and environmental factors. What you eat plays a significant role in determining your risk of developing this condition. While it’s known that a diet rich in plant-based foods can reduce the risk of FLD, not all plant-based foods are equal in this regard. Refined grains, sugar-sweetened beverages, and fruit juices can actually increase your risk.
However, many studies on this topic have had limitations, including small sample sizes, which made it hard to fully understand the impact of diet on FLD. One recent study aimed to fill that gap by analyzing data from a large group of participants in the United Kingdom.
The Study: What We Know
This longitudinal study collected data from over 500,000 participants in England, Scotland, and Wales, aged 37 to 73. The researchers excluded those already diagnosed with FLD, cirrhosis, other liver diseases, or alcohol-related problems. They also excluded individuals with incomplete genetic data or who weren’t of European descent.
To understand the participants’ diets, the researchers used a dietary recall questionnaire called the Oxford WebQ. They categorized various foods into groups, which fell into three main categories: healthy plant-based foods, less healthy plant-based foods, and animal-based foods. They then calculated different plant-based diet indices (PDIs) based on the participants’ dietary choices.
What Did They Find?
The study included 159,222 participants in the FLD risk analysis and 20,692 in the liver fat content analysis. These participants were, on average, 58 years old, with 58% of them being female.
The researchers found that a higher consumption of plant-based foods, particularly those in the healthy plant-based diet index (hPDI), was associated with a lower risk of FLD and lower liver fat content. Some examples of hPDI include- Whole grains like bran cereal, brown rice, whole wheat cereal, fruits, vegetables, salted and unsalted peanuts, legumes including baked beans, green beans, peas, tofu, tea and coffee etc.
In contrast, a higher consumption of less healthy plant-based foods (uPDI) increased the risk of FLD and liver fat content. These include refined grains such as oat crunch, sweetened cereal, white bread, white pasta, white rice, sweet potato, potatoes, carbonated drinks, fruit juices, sweets and desserts.
Additionally, the study found that improving diet quality, like following a Mediterranean diet, influenced the genetic risk of FLD. This suggests that what you eat can modify your genetic susceptibility to FLD.
The Power of Plant-Based Foods
Specific plant-based foods like nuts, tea, and coffee were associated with a reduced risk of FLD. These foods are rich in nutrients like flavonoids, dietary fiber, caffeine, phytosterols, and plant proteins. These compounds can improve insulin resistance, gut health, and reduce central obesity, all of which contribute to a lower risk of FLD.
Conclusion: Diet Matters, Genetics too
While this study has some limitations, it highlights the crucial interplay between genetics and diet in influencing FLD risk. Eating a diet rich in healthy plant-based foods can reduce your risk of FLD, regardless of your genetic makeup. Conversely, consuming less healthy plant-based foods can increase your risk.
This research underscores the importance of adopting a healthy plant-based diet to protect yourself from FLD, even if you have genetic predispositions. So, if you’re looking to safeguard your liver health, remember to load up on those leafy greens, nuts, and other plant-based goodies – your liver will thank you!
#FattyLiver #healthyliving #fitness #healthyeating #plantbaseddiet
- Lv, Y., Rong, S., Deng, Y., et al. (2023) Plant-based diets, genetic predisposition and risk of non-alcoholic fatty liver disease. BMC Medicine 21(351). doi:10.1186/s12916-023-03028